Glaucoma
is leading towards the second most common cause of worldwide irreversible
blindness1 and approximately sixty million people are suffering from
glaucoma globally1,2. Glaucoma therapies are designed to either
increase the outflow or decrease the production of aqueous humor in order to
reduce intraocular pressure (IOP) and preserve visual function3.
Studies have shown that reducing intraocular pressure helps to preserve visual
function in most cases3. Surgical intervention is needed when
medication fails to control intraocular pressure (IOP), which is required to
preserve optic nerve function4. Current glaucoma therapies include
topical medications, laser therapies, microinvasive glaucoma surgery, and
incisional glaucoma surgery. Most therapies are designed to reduce the
production of aqueous humor, increase uveoscleral outflow or both5.
Trabeculectomy with or without
anti-metabolites, and glaucoma drainage devices are considered to be the
initial IOP lowering surgical procedures followed by6 Cycloablation,
in which destruction of ciliary body epithelium and stroma is done, thus
reducing aqueous production7. Cyclo G6 system with MP3 probe,
deliver microsecond thermal energy that is confined to target tissue,
preventing destruction of surrounding tissue by on and off cycles mode,
allowing energy to build up in the targeted pigmented tissues, reaching to
coagulative threshold7.
In Ten et al study the mean preoperative
IOP was 39.3 ± 12.6 mm Hg that decreased to 31.1 ± 13.4 mm Hg, 28.0 ± 12.0 mm Hg,
27.4 ± 12.7 mmHg, 27.1 ± 13.6 mm Hg, 25.8 ± 14.5 mm Hg, 26.6 ± 14.7 mm Hg and
26.2 ± 14.3 mm Hg at 1st day, 1st week, 1, 3, 6, 12 and 18 months
respectively. After a mean of 1.3 treatment sessions, success achieved was
72.7%8. Numerous studies have demonstrated the efficacy and high
safety profile of micro pulse trans-scleral cyclophotocoagulation MP-TSCPC in
refractory glaucomas9-14. Reduction of mean IOP was seen in 60.3% at
1 week and 33.4% at 1 month. The procedure was safe in all cases and
effectiveness was found in 71% of the patients15.
There are few
international studies in literature describing the clinical outcomes of
micropulsed mp3 cyclodiode laser, in which the work is mostly done in patients
with advanced glaucoma with no local studies. The aim of this study is to
consider MP3 cyclodiode laser for other glaucoma patients, to control
intraocular pressure with the reduction of number of treatments especially
excluding the oral acetazolamide to minimize collateral damage, unwanted side
effects and to overcome the unavailability of this drug in Pakistan.
MATERIAL AND METHODS
This descriptive case
series was conducted from 15.03.19 to 15.09.19 at Liaquat National Hospital,
Karachi in the department of ophthalmology after the approval of ethical
committee. WHO sample size calculator was used to calculate sample size. All
patients of either gender with age 20 to 50 years having Primary open angle
glaucoma, Neovascular, Refractory, Uveitic, Trauma induced glaucoma, and Post
vitrectomy induced glaucoma were included in the study. Patients with Primary
angle closure and Normal tension glaucoma were excluded from the study.
Clinical history was recorded. Informed written
consent was taken before enrolment. Data was collected using a proforma, which
included age, gender, duration of glaucoma, number of anti-glaucoma
medications, visual acuity using Snellen chart and intraocular pressure with the
Goldmann Applanation tonometer. Type of glaucoma was labeled after slit lamp
examination. The Micro pulse trans-scleral cyclophotocoagulation (MPTSCPC)
diode laser procedure was performed after injecting retro bulbar anesthesia of
3-5ml of lidocaine. Cyclo G6 laser system (IRIDEX laser system) which uses a
laser diode of 810 nm infrared wavelength with MP3 probe was used. Treatment
was done using total duration of 1.6 millisecond (ms) including 0.5 millisecond
on time, 1.1 ms off time, 31.33% duty cycle and power of 2000 mW. Globe
manipulation by cotton swabs and placement of speculum was censured by adequate
exposure to the targeted area. The laser probe was positioned perpendicular to
the surface of the globe with fiberoptic tip 3 mm away from the limbus. Laser
application was done to the upper and lower hemisphere in “painting” direction,
avoiding the 3 and 9 o’clock positions to avoid risk of damage to the
neurovascular bundles. The laser was delivered for 80 seconds for superior and
inferior hemisphere for a total of 160 seconds of treatment. Patients received
post-operative dose of dexamethasone ointment and were patched for 1 hour. All
patients were started on topical Moxifloxicin, Fluoromethalone and neomycin one hourly and after 1 week tapered
to 4 times a day. The following baseline parameters were collected for each
visit at 1 week, 1 month and 3 months. Intraocular pressure, number of
anti-glaucoma medications used including oral acetazolamide and any
complications were recorded. Topical anti-glaucoma medications were tapered or
adjusted at the doctor’s discretion. Effectiveness of the procedure of the
treated eyes was defined as reduction of IOP by 30% from baseline IOP after 1
month follow up or withdrawal of oral acetazolamide.
SPSS version 22 was used
for data compilation and analysis. Frequencies and percentages were computed
for categorical variables. Quantitative variables were presented as mean ± standard
deviation. The mean baseline IOP was compared with mean IOP at 3 months using
student t test. Effect modifiers were controlled through stratification.
Post-stratification chi square and fisher exact test was used to see the
association of effectiveness with stratified groups. Repeated measures of ANOVA
were applied to compare means. P value ≤0.05 was considered level of
significance.
RESULTS
Ninety-eight cases were included in study.
Out of whom 62 (63.3%) were males and 36 (36.7%) were females. The descriptive
statistics including mean age of the patients, type of glaucoma, side of
treatment, quadrants treated are given in Table 1. Effectiveness of treatment
was seen in 85.7% cases. We found insignificant association of effectiveness
with gender (p = 0.199), age groups (p = 0.096), type (p = 0.656) and procedure
(p = 0.231) as shown in Table-2.
Mean pre-op IOP, after 1 week, 1 month and
3 months for unilateral and bilateral cases is shown in Table-3. Acetazolamide
was not given to 35(35.7%) cases while stopped for 53 (54.1%) cases and
10(10.2%) cases continued with acetazolamide.
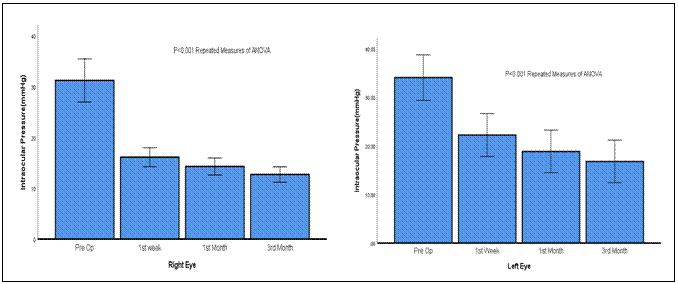
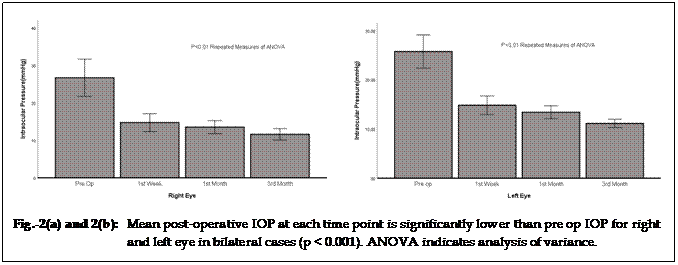
Mean post-operative IOP at each time point
was significantly lower than pre op IOP for unilateral (right and left eye) and
bilateral (right and left eye) cases as shown in Figure 1 (a), Figure 1 (b),
Figure 2 (a) and Figure 2 (b). Significant mean difference was found for pre-op
IOP with IOP after 3 months for unilateral right eye (p = 0.000), unilateral
left eye (p = 0.00), Bilateral right eye (p = 0.000) and Bilateral left eye ( p
=0.000) as presented in Table-4.
Our complications which
were generally tolerated well were conjunctival hemorrhage because of the tip
of the probe, which resolved later. The most significant but rare side effect seen
was severe surface epithelial erosion all over cornea and it took 3-6 weeks to
come back to normal with Autologus serum. In one patient, permanent central scar was
formed because of infection. Four to five patients did not respond to treatment
even after repeating the procedure after 3 months. We could not explain this
phenomenon.
Table 1: Descriptive statistics
of study population.
|
|
n(%)
|
|
Age(years)˚
|
|
48.46 ± 13.39
|
|
Gender
|
Male
|
62 (63.3)
|
|
Female
|
36 (36.7)
|
|
Number of Drops
|
0 to 0
|
1 (1)
|
|
1 to 1
|
16 (16.3)
|
|
2 to 0
|
9 (9.2)
|
|
2 to 1
|
11 (11.2)
|
|
2 to 2
|
22 (22.4)
|
|
3 to 0
|
6 (6.1)
|
|
3 to 1
|
8 (8.2)
|
|
3 to 2
|
17 (17.3)
|
|
3 to 3
|
7 (7.1)
|
|
4 to 2
|
1 (1)
|
|
AZM
|
Stop
|
53 (54.1)
|
|
Continue
|
10 (10.2)
|
|
Not Given
|
35 (35.7)
|
|
Type
|
Chronic
|
18 (18.4)
|
|
Neovascular
|
4 (4.1)
|
|
Refractory
|
28 (28.6)
|
|
Trauma
|
14 (14.3)
|
|
Uveitic
|
6 (6.1)
|
|
Vitrectomy
|
28 (28.6)
|
|
Eye
|
Right
|
36 (36.7)
|
|
Left
|
36 (36.7)
|
|
Both
|
26 (26.5)
|
|
Procedure
|
180
|
34 (34.7)
|
|
360
|
64 (65.3)
|
|
Effectiveness
|
Yes
|
84 (85.7)
|
|
No
|
14 (14.3)
|
|
Mean ± SD
|
|
|
Table 2: Association of effectiveness with population characteristics.
|
|
Effectiveness
|
P-value
|
|
Yes
|
No
|
|
Gender
|
Male
|
51 (60.7)
|
11 (78.6)
|
0.199
|
|
Female
|
33 (39.3)
|
3 (21.4)
|
|
Age Group
|
≤50 years
|
34 (40.5)
|
9 (64.3)
|
0.096
|
|
>50 years
|
50 (59.5)
|
5 (35.7)
|
|
Type↨
|
Chronic
|
16 (19)
|
2 (14.3)
|
0.656
|
|
Neovascular
|
4 (4.8)
|
0 (0)
|
|
Refractory
|
25 (29.8)
|
3 (21.4)
|
|
Trauma
|
11 (13.1)
|
3 (21.4)
|
|
Uveitic
|
4 (4.8)
|
2 (14.3)
|
|
Vitrectomy
|
24 (28.6)
|
4 (28.6)
|
|
Procedure↨
|
180 degree
|
27 (32.1)
|
7 (50)
|
0.231
|
|
360 degree
|
57 (67.9)
|
7 (50)
|
|
Chi Square test was applied.
|
|
↨Fisher exact test was applied.
|
|
P≤0.05, considered as significant.
|
DISCUSSION
Cyclo photocoagulation (CPC) with
MicroPulse 3 device represents a new tissue-sparing technology used for simple
as well as for complex glaucoma15. Standard coagulation involves
ciliary body epithelium and stroma destruction by targeting it, resulting in
decreased aqueous secretion and eventually IOP control. As compared to
conventional CPC which delivers continuous, high intensity energy, MP3 delivers
repetitive short pulse laser energy series followed by rest period8,15,16-18.
Complications related to cyclodestruction procedure includes vision loss,
pupillary distortion, corneal edema, cystoid macula, hypotony, and edema19,20.
Micro pulse MP3 cyclophotocoagulation
showed effectiveness for 85.7% of the cases in our study which is nearly same
as reported by Kareen Zaroor (81.7%)21. Yelenskiy A reported 71%
effectivness.19 Success rate varies from 40% to 80% in different
studies22-24.
The advent of micro-pulsed trans-scleral
diode laser has revolutionized diode laser as well as other laser types, even
CO2 laser. Concept of micro-pulsing allows maximum effectiveness by
generating significant amounts of energies to reach target tissues and allowing
time for heat to diffuse instead of building up, to reduce the risk of unwanted
side effects and to make this laser safe and predictable enough to use in seeing
eyes1. The procedure is well-known for its ease, non-invasiveness
and well toleration. Bleeding and postoperative infection risks are eliminated
by trans-scleral application. At every level of the glaucoma spectrum, MP3 is
shown as safe and effective procedure for affected eyes1.
Excellent safety profile is documented with
this treatment. One of the recent studies also reported very good results of
the procedure with no complications (i.e. phthisis bulbi, hypotony and macular
edema).6 In our study, we found significant mean difference for
pre-op IOP with IOP after 3 months for right eye (p = 0.000) and left eye (p = 0.00).
Emanuel et al. showed higher reduction of IOP24, this has been
attributed both to the possibility of increased uveoscleral outflow, as well as
decreased aqueous production22.
Emanuel et al also reported reduction in
the need of topical eye drops21. Other studies also reported lesser
need of number of eye drops10. However, it is noteworthy that in 54%
of the patients in our study we were able to withdraw acetazolamide tablets, a
treatment that was not used in other studies1,16,24. This could
explain the reason why the number of hypotensive drops did not decrease as
drastically as reported in other studies24.
The limitation of our
study is the short-term follow up but we are continuing our study for long term
follow-up. Previously, cyclodestructive procedures such as cyclocryotherapy and
CPC were reserved for poorly controlled glaucoma, limited visual prognosis and
mainly retained for end stage glaucoma, because of associated complication with
cyclodestructive procedures that include vision loss, corneal edema, pupillary
distortion, cystoid macula edema, and hypotony19. We did not notice
any significant complications following MP-TSCPC in our study. Tan et al found
MP-TSCPC comparable to conventional TSCPC with potentially lower rate of
complication23.
CONCLUSION
This new method of
micropulse delivery may be of help in patients who cannot take medications or
want to delay incisional surgery. Micro pulse MP3 can thus be a viable option
in patients with prior failed filtering surgery, given the fact that repetition
of incisional glaucoma procedures can be technically demanding and fraught with
complications, not to mention the lower success rates of glaucoma reoperations.
Micro pulse MP3 provides promising results with high level of effectiveness and
with great potential advantages to be considered as a safe alternative
procedure.
CONFLICT OF INTEREST
None
REFERENCES
1.
Toyos MM, Toyos R. Clinical outcomes of micropulse transcleral cyclophotocoagulation
in moderate to severe glaucoma. J Clin Exp Ophthalmol. 2016; 7 (620): 2.
2.
Quigley HA, Broman AT. The number of people with glaucoma worldwide in
2010 and 2020. Br J Ophthalmol. 2006; 3: 262–7.
3.
Weinreb RN, Khaw PT. Primary open-angle glaucoma. The Lancet. 2004;
363 (9422):1 711-20.
4.
Lai JS, Tham CC, Lam DS. Surgical management of chronic closed angle
glaucoma. Asian Pac J Ophthalmol. 2003; 15: 5–10.
5.
Nguyen QH. Primary surgical management refractory glaucoma:
tubes as initial surgery. Curr Opin Ophthalmol. 2009; 20: 122–5.
6.
Noecker RJ, Kelly T, Patterson E, Herrygers LA. Diode laser contact trans-sclera
cyclophotocoagulation: getting the most from the G – probe. Ophthalmic Surg
Lasers Imaging, 2004; 35: 124–30.
7.
Abdelrahman AM. Refractory Glaucomas. Types and Management. J
Ophthalmol related Sci. 2017; 1 (1): 1-14.
8.
Aquino MC, Barton K, Tan AM, Snq C, Li X, Loon
SC, et al. Micropulse
versus continuous wave transscleral diode cyclophotocoagulation in refractory
glaucoma: a randomized exploratory study. Clin Exp Ophthalmol. 2015; 43 (1): 40-46.
9.
Radcliffe N, Vold S, Kammer J. Micropulse transscleral cyclophotocoagulation
(mTSCPC) for the treatment of glaucoma using the Micro Pulse P3 device. Am
Glaucoma Soc annual meeting. 2015.
10.
Kuchar S, Moster M, Waisbourd M. Treatment outcomes of Micro Pulse trans-scleral
cyclophotocoagulation advanced glaucoma. Am Glaucoma Soc annual meeting, 2015.
11.
Resende A, Waisbourd M, Amarasekera D. A prospective pilot study evaluating the novel Micropulse
transscleral cyclophotocoagulation: short-term results. Am Glaucoma Soc annual
meeting, 2016.
12.
Lin S, Babic K, Masis M. Micropulse transscleral diode laser
cyclophotocoagulation: short term results and anatomical effects. Am Glaucoma
Soc annual meeting, 2016.
13.
Maslin JS, Chen P, Sinard J, Noecker R. Comparison of acute histopathological changes in
human cadaver eyes after MicroPulse and continuous wave transscleral cyclophotocoagulation.
Am Glaucoma Soc annual meeting, 2016.
14.
Maslin J, Noecker R. Micropulse trans-scleral cyclophotocoagulation
for the treatment of glaucoma. Assoc Res Vision Ophthalmol. 2016.
15.
Gavris MM, Olteanu I, Kantor E, Mateescu R,
Belicioiu R. IRIDEX
MicroPulse P3: innovative cyclophotocoagulation. Romanian J Ophthalmol. 2017; 61
(2): 107.
16.
Tan AM, Chockalingam M, Aquino MC, Lim Zl, See JL,
Chew PT. Micropulse
trans-scleral diode laser cyclophotocoagulation in the treatment of refractory
glaucoma. Clin Exp Ophthalmol. 2010; 38 (3): 266-72.
17.
Sivaprasad S, Sandhu R, Tandon A, Sayed Ahmed K,
McHugh DA.
Subthreshold micropulse diode laser photocoagulation for clinically significant
diabetic macular oedema: a three‐year follow up. Clin Exp Ophthalmol. 2007; 35 (7): 640-4.
18.
Parodi MB, Di Stefano G, Ravalico G. Grid laser treatment for exudative retinal
detachment secondary to ischemic branch retinal vein occlusion. Retina. 2008; 28
(1): 97-102.
19.
Yelenskiy A, Gillette TB, Arosemena A, Stern AG,
Garris WJ, Young CT, et al. Patient Outcomes Following Micropulse Transscleral Cyclophotocoagulation:
Intermediate-term Results. J glaucoma. 2018; 27 (10): 920-5.
20.
Vernon SA, Koppens JM, Menon GJ, Negi AK. Diode laser cycloablation in adult glaucoma:
long‐term results of a standard protocol and review of current
literature. Clin Exp Ophthalmol. 2006; 34 (5): 411-20.
21.
Zaarour K, Abdelmassih Y, Arej N, Cherfan G,
Tomey KF, Khoueir Z. Outcomes of Micropulse Transscleral Cyclophotocoagulation in
Uncontrolled Glaucoma Patients. J Glaucoma. 2019; 28 (3): 270-5.
22.
Kuchar S, Moster MR, Reamer CB, Waisbourd M. Treatment outcomes of micropulse transscleral cyclophotocoagulation
in advanced glaucoma. Lasers Med Sci. 2016; 31 (2): 393-6.
23.
Aquino MC, Barton K, Tan AM, Sng C, Li X, Loon
SC, et al.
Micropulse versus continuous wave transscleral diode cyclophotocoagulation in
refractory glaucoma: a randomized exploratory study. Clin Exp Ophthalmol. 2015;
43 (1): 40-6.
24.
Emanuel ME, Grover DS, Fellman RL, Godfrey DG,
Smith O, Butler MR, et al. Micropulse cyclophotocoagulation: initial results in
refractory glaucoma. J Glaucoma. 2017; 26 (8): 726-9.